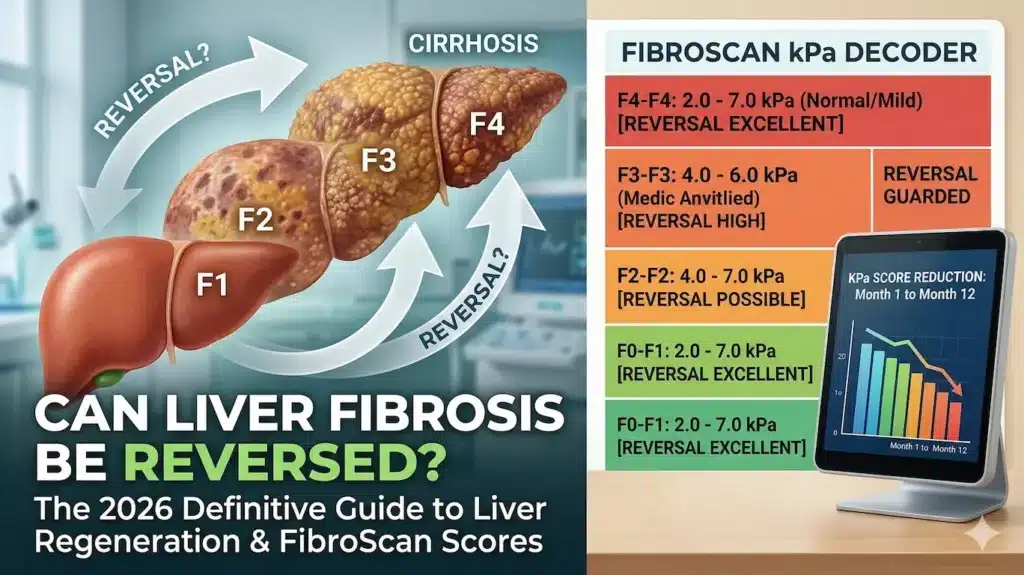
Can Liver Fibrosis Be Reversed? The 2026 Definitive Guide to Liver Regeneration
For years, a diagnosis of liver fibrosis felt like a one-way street toward cirrhosis. Medical textbooks often described liver scarring as permanent, leaving patients to simply “manage” the decline. But as we move through 2026, the clinical reality has changed. If you are asking,
“Can liver fibrosis be reversed?” the answer is a resounding yes—but with a significant caveat. Reversal is not a passive process of waiting; it is a biological “race” between the deposition of scar tissue and your liver’s innate ability to dissolve it.
While your liver is the only organ capable of true regeneration, the “point of no return” is much further along than we once thought. However, simply “eating better” isn’t enough to break down existing collagen fibers. You need a specific metabolic environment and, in many cases, targeted pharmacological intervention to flip the switch from fibrogenesis (scarring) to fibrolysis (scar breakdown). In this 1,800-word deep dive, we reveal the 2026 protocols that are successfully moving patients from Stage F3 back to Stage F1 and F0.
Understanding the Stages: F0 to F4
To understand reversal, you must know where you stand on the METAVIR scale. Fibrosis is the liver’s “healing” response to chronic injury—whether from fat, alcohol, or virus.
- F0-F1: Minimal scarring. Reversal is almost guaranteed with the removal of the underlying cause.
- F2: Moderate scarring. The architecture of the liver is starting to change, but reversal is still highly probable.
- F3: Advanced fibrosis (bridging fibrosis). This is the “danger zone” just before cirrhosis. Reversal is still possible but requires aggressive intervention.
- F4: Cirrhosis. While complete reversal is rare, modern 2026 therapies focus on “recompensating” the liver to prevent failure.
While managing inflammation is the first step, understanding the structural timeline of healing is vital; for more details on recovery, see our guide on.
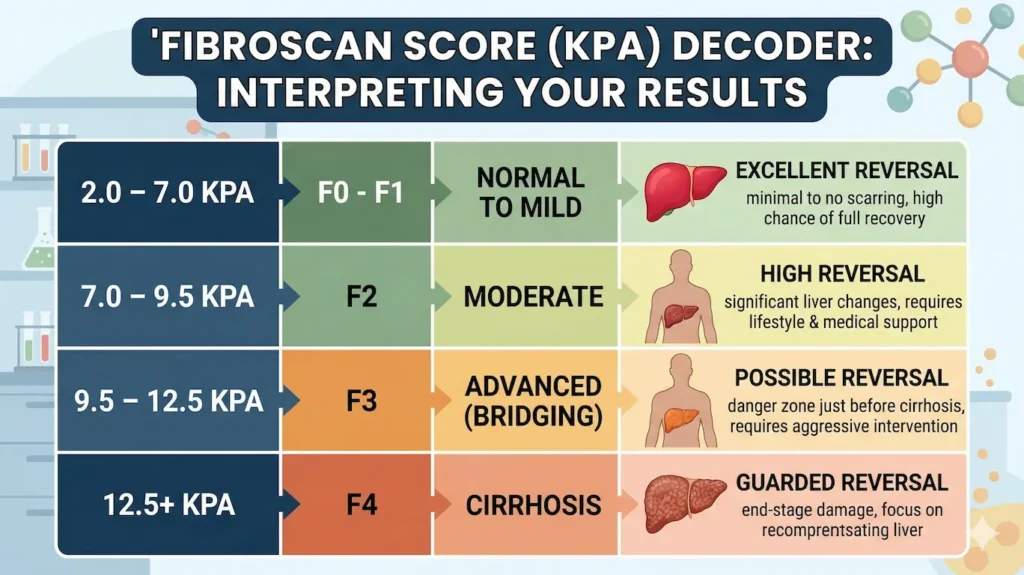
The 2026 FibroScan Score (kPa) Decoder Chart
This chart helps translate your Liver Stiffness Measurement (LSM) into a METAVIR fibrosis stage. Please note that “normal” ranges can vary slightly depending on whether the underlying cause is MASH, Hepatitis, or Alcohol.
| FibroScan Score (kPa) | Fibrosis Stage | Severity Level | Reversal Potential |
| 2.0 – 7.0 kPa | F0 – F1 | Normal to Mild | Excellent: Reversal is highly likely with basic lifestyle changes. |
| 7.0 – 9.5 kPa | F2 | Moderate | High: Targeted diet and GLP-1 therapy show rapid results here. |
| 9.5 – 12.5 kPa | F3 | Advanced (Bridging) | Possible: Requires aggressive 2026 protocols (Resmetirom + Weight Loss). |
| 12.5+ kPa | F4 | Cirrhosis | Guarded: Focus shifts to “recompensation” and preventing failure. |
How to Read Your CAP Score (Steatosis)
Often, a FibroScan report also includes a CAP score (measured in dB/m). While the kPa score measures scarring, the CAP score measures fat.
- S1 (Mild): 238–260 dB/m
- S2 (Moderate): 260–290 dB/m
- S3 (Severe): >290 dB/m
3 Tips for an Accurate FibroScan Result
- Fast for 3+ Hours: Eating before a scan can artificially inflate your kPa score by increasing blood flow to the liver.
- Check the “IQR/med” Ratio: For a scan to be reliable, the IQR/med ratio should be less than 30%. If it’s higher, the result may be inaccurate due to technical interference.
- Mind the Inflammation: If your ALT enzymes are currently very high (acute inflammation), your FibroScan might “overestimate” your fibrosis. Always look at your blood work and scan results together.
The Biological Mechanism of Reversal
Reversing fibrosis requires two simultaneous actions: stopping the activation of Hepatic Stellate Cells (HSCs) and activating Matrix Metalloproteinases (MMPs). HSCs are the “architects of scarring.” When the liver is injured, these cells turn into myofibroblasts and pump out collagen. To reverse the damage, we must return these cells to their “quiescent” or dormant state.
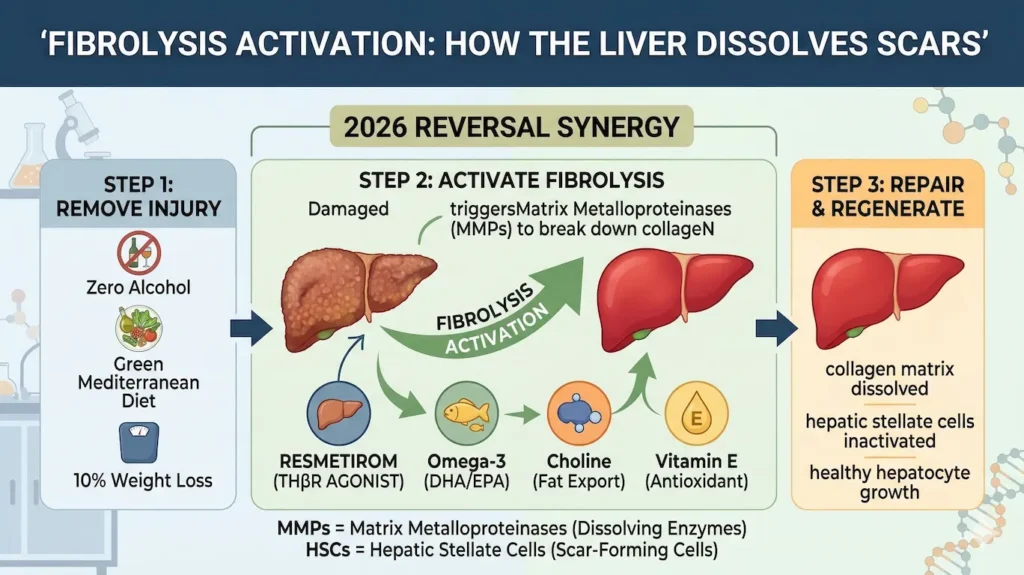
The 2026 Reversal Protocol: Drugs and Nutrients
In 2026, the treatment of fibrosis has moved beyond simple monitoring. We now use a “Multi-Hit” approach.
1. Targeted Anti-Fibrotics
Drugs like Resmetirom (Rezdiffra) are now standard for Stage F2 and F3 patients. By activating thyroid hormone receptors in the liver, Resmetirom reduces the fat that fuels the inflammation, allowing the liver’s natural “cleaning” enzymes to break down existing scars.
2. The Role of GLP-1 Agonists
While technically weight-loss drugs, Semaglutide and Tirzepatide have shown a massive “off-label” success in fibrosis reversal. By achieving a 10% body weight loss, patients reduce the mechanical pressure on liver cells, which signals the HSCs to stop producing collagen.
3. Nutrient Synergists
- Vitamin E (High Dose): Acts as a shield for the hepatocytes, preventing the cell death that triggers new scars.
- Coffee (3 Cups Daily): The polyphenols in coffee are now medically recognized to interfere with the signaling pathways of scar-forming cells.
The Timeline: How Long Does Reversal Take?
Liver regeneration is a marathon. Clinical data from 2026 suggests that while liver enzymes (ALT/AST) can normalize in weeks, actual structural reversal of scar tissue takes 12 to 24 months of consistent adherence to the protocol. Most patients see a significant improvement in their FibroScan (KPa) scores after one year of targeted treatment.
Common Pitfalls: Why Some Fibrosis Doesn’t Reverse
The most common reason for reversal failure is “Hidden Triggers.” Even if a patient stops drinking or loses weight, high intake of concentrated fructose or chronic exposure to environmental toxins (like mold or heavy metals) can keep HSCs in an activated state.
FAQ: Can Liver Fibrosis Be Reversed
1. Can Stage 3 liver fibrosis be reversed?
Yes, Stage 3 liver fibrosis (F3) is considered reversible in 2026. Clinical studies show that by combining a 10% weight loss with FDA-approved MASH medications like Resmetirom, the liver can dissolve bridging fibrosis and return to earlier, healthier stages (F2 or F1).
2. How long does it take to reverse liver fibrosis?
The timeline for liver fibrosis reversal typically ranges from 12 to 24 months. While blood markers (liver enzymes) may improve in 3 months, the physical breakdown of collagen scar tissue requires a long-term, stable metabolic environment.
3. What is the best medication for reversing liver scarring?
As of 2026, Resmetirom (Rezdiffra) is the primary FDA-approved medication specifically indicated to improve liver fibrosis. Additionally, GLP-1 agonists like Tirzepatide are highly effective at resolving the inflammation that causes scarring.
4. Can you reverse liver fibrosis naturally?
Early-stage fibrosis (F1-F2) can often be reversed naturally through a Green Mediterranean diet, total alcohol abstinence, and achieving 7-10% weight loss. These actions remove the triggers for scar formation, allowing the liver to regenerate.
5. Is liver fibrosis the same as cirrhosis?
No. Fibrosis is the process of scarring, while cirrhosis (Stage F4) is the end-stage result where the scarring is so extensive it disrupts liver function and blood flow. Fibrosis is highly reversible; cirrhosis is much more difficult to reverse.
6. Does coffee help reverse liver fibrosis?
Yes. Medical research indicates that drinking 3 cups of black coffee per day can slow the progression of liver scarring and assist in the reversal process by inhibiting the activation of scar-producing stellate cells.
7. What is a “good” FibroScan score for reversal?
A FibroScan score (measured in kPa) below 7.0 generally indicates minimal fibrosis (F0-F1). Scores between 9.5 and 12.5 indicate Stage F3, where reversal protocols should be aggressively implemented to prevent F4 cirrhosis.
5 Medical Sources & Citations
- Mayo Clinic: Liver Fibrosis Stages and Treatment Options
- The Lancet: Regression of Liver Fibrosis: Clinical Evidence and Future Directions
- National Institutes of Health (NIH): Cellular Mechanisms of Liver Fibrosis Reversal
- American Liver Foundation: Can You Reverse Liver Damage?
- AASLD: 2026 Guidelines on MASH and Fibrosis Management
Medical Disclaimer: The information provided in this article is for informational purposes only and does not constitute medical advice. Always consult with a hepatologist or a qua