GLP-1 Injections Explained: How They Work for Weight Loss & Diabetes

Imagine a medication that not only lowers blood sugar but also helps you lose a significant amount of weight — and may even protect your heart. That’s exactly what GLP-1 injections are doing for millions of people right now.
In 2026, these treatments have moved from niche diabetes care into mainstream medicine, with over 30 million Americans currently using them [2].
Whether you’re managing type 2 diabetes, struggling with obesity, or simply trying to understand what all the buzz is about, this guide breaks it all down clearly.
Key Takeaways 🔑
- GLP-1 injections mimic a natural gut hormone to lower blood sugar, reduce appetite, and promote weight loss.
- Originally developed for type 2 diabetes, these medications are now widely approved for chronic weight management.
- Clinical trials show weight loss ranging from 13% to over 20% of body weight depending on the drug and dose.
- New formulations — including higher-dose injectables and oral options — are expanding access in 2026.
- GLP-1 therapies also offer significant cardiovascular benefits beyond just weight and blood sugar control.
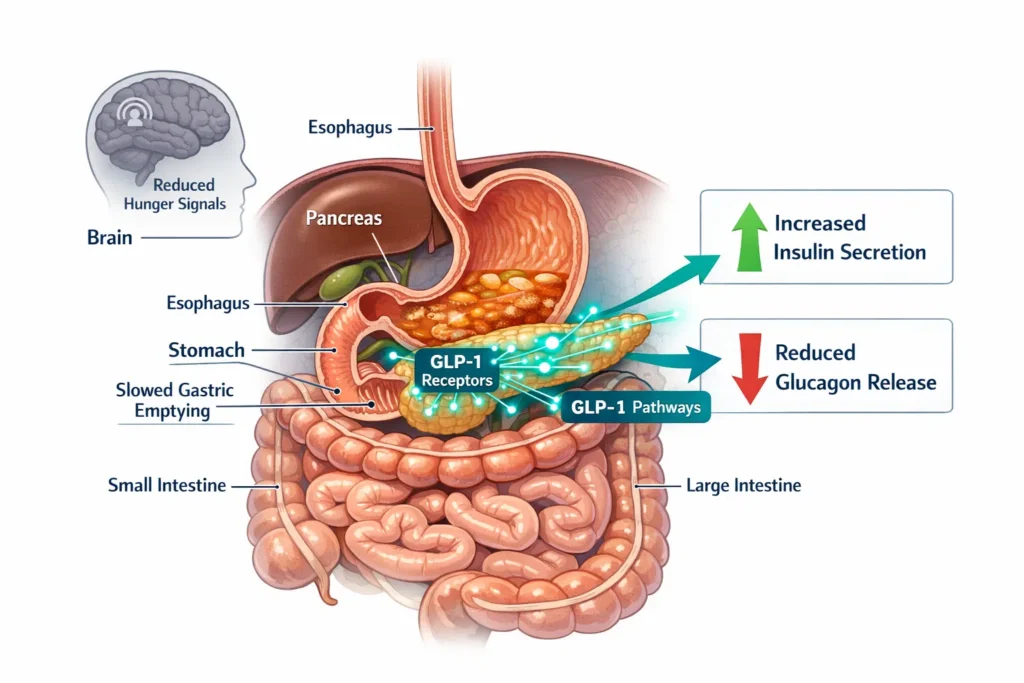
How GLP-1 Injections Work: The Science Made Simple
What Is GLP-1?
GLP-1 stands for glucagon-like peptide-1. It’s a hormone your gut naturally releases after you eat. Think of it as a signal that tells your body: “Food is here — manage it wisely.”
GLP-1 receptor agonists are medications that mimic this hormone. When injected (or taken orally), they bind to GLP-1 receptors throughout the body and trigger several helpful responses [1][5]:
- 🩺 Increase insulin secretion — helps lower blood sugar after meals
- 🚫 Decrease glucagon — stops the liver from releasing excess sugar
- 🐢 Slow gastric emptying — food moves through your stomach more slowly, keeping you fuller longer
- 🧠 Reduce appetite — signals the brain to feel satisfied sooner
“GLP-1 receptor agonists work on multiple systems at once — the pancreas, the liver, the stomach, and the brain. That’s what makes them so effective.”
Originally a Diabetes Drug — Now Much More
GLP-1 medications were first developed to treat type 2 diabetes. Their ability to lower blood sugar without causing dangerous hypoglycemia (low blood sugar) made them a major breakthrough [5]. But researchers quickly noticed something else: patients were also losing significant weight.
That observation changed everything. Today, GLP-1 drugs are approved for:
| Condition | Examples of Approved GLP-1 Drugs |
| Type 2 Diabetes | Ozempic (semaglutide), Trulicity (dulaglutide) |
| Chronic Weight Management | Wegovy (semaglutide), Zepbound (tirzepatide) |
| Cardiovascular Risk Reduction | Wegovy (semaglutide) |
The Cardiovascular Bonus 💓
One of the most exciting findings is that GLP-1 injections provide heart benefits independent of weight loss.
Research from Harvard Medical School found that GLP-1 medications delivered a 40% relative risk reduction for patients with heart failure with preserved ejection fraction compared to older diabetes medications — a result described as something you don’t see with every drug [4].
This makes them valuable even for patients whose primary concern isn’t weight.
GLP-1 Injections for Weight Loss: What the Data Shows
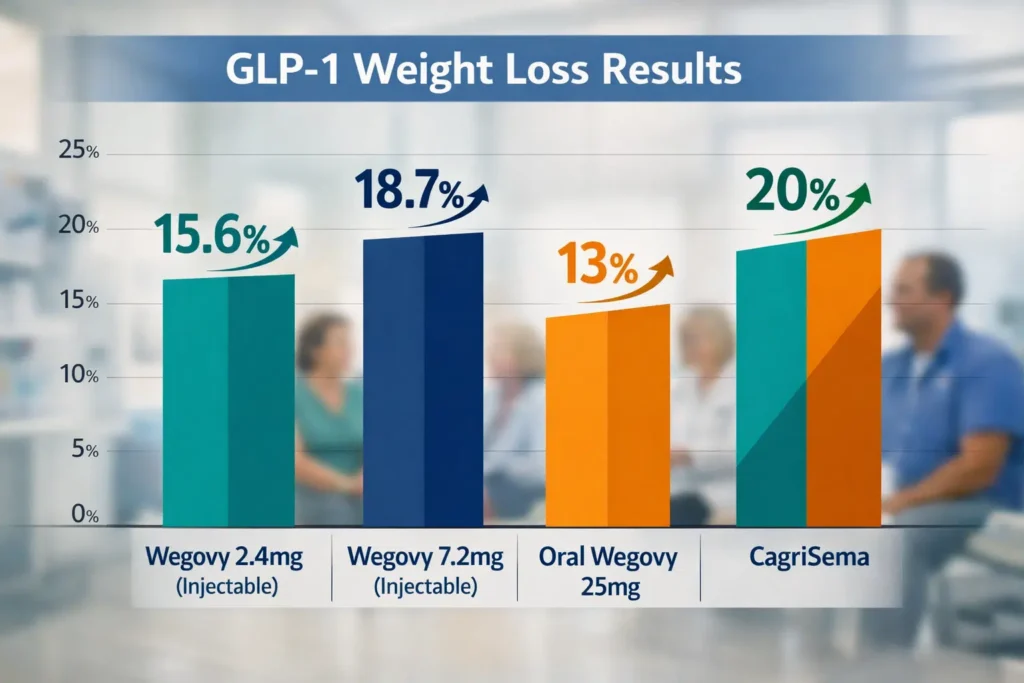
How Much Weight Can You Actually Lose?
The results from clinical trials are impressive — and getting better with each new generation of drugs. Here’s a clear breakdown of what the evidence shows:
| Medication | Format | Weight Loss | Trial Duration |
| Wegovy 2.4 mg | Weekly injection | ~15.6% | 72 weeks |
| Wegovy 7.2 mg (pending FDA) | Weekly injection | 18.7% | 72 weeks |
| Oral Wegovy 25 mg | Daily pill | ~13% | 64–68 weeks |
| Tirzepatide (Zepbound) | Weekly injection | ~20–22% | 72 weeks |
| CagriSema (in trials) | Weekly injection | ~20–23% | 68 weeks |
Sources: [1][2][3]
💡 Key insight: Participants who stayed on the 7.2 mg injectable Wegovy for the full trial lost nearly 21% of their starting body weight [3]. For a 250-pound person, that’s roughly 52 pounds.
Injectable vs. Oral GLP-1 Medications
A big question in 2026 is: Do you need the injection, or can a pill work just as well?
The honest answer is that injectable GLP-1 injections remain more effective than oral alternatives. People using injectable Wegovy lost an average of 15–16% of body weight, compared to 13% with oral Wegovy 25 mg over similar time periods [2]. That said, oral options are a game-changer for people who are needle-averse or face access barriers.
Oral semaglutide (Wegovy pill) became the first oral GLP-1 approved for weight loss on December 22, 2025. Within just three weeks of its January 5, 2026 U.S. launch, approximately 170,000 prescriptions were filled — outpacing the early adoption of every previous GLP-1 medication [1][2].
Eli Lilly’s orforglipron (36 mg daily) is another oral option awaiting FDA approval by Q2 2026. It showed 11.2% mean weight loss at 72 weeks in the ATTAIN-1 trial — slightly less than injectables, but still meaningful for a once-daily pill [1].
Who Benefits Most? 👥
A major Johns Hopkins analysis found that GLP-1 medications work comparably across age groups, racial backgrounds, and starting body weight [6]. This is important — it means these drugs aren’t just effective for one type of patient.
However, there is a notable gender difference:
- 👩 Women lost an average of 11% of starting weight
- 👨 Men lost an average of 7% of starting weight [6]
Researchers are still studying why this gap exists, but it doesn’t mean the drugs are ineffective for men — both groups saw clinically meaningful results.
What’s Coming Next in 2026? 🔭
The GLP-1 landscape is moving fast. Three major FDA decisions are expected in 2026 [1]:
- Wegovy 7.2 mg injectable — higher-dose semaglutide for greater weight loss
- Orforglipron (Eli Lilly) — once-daily oral option, expected Q2 2026 approval
- CagriSema — a combination injectable (cagrilintide + semaglutide) being compared head-to-head against tirzepatide in a trial wrapping up this year [3]
These new options could make GLP-1 therapy more accessible, more effective, and better tailored to individual needs.
Common Questions About GLP-1 Injections
Are GLP-1 Injections Safe?
GLP-1 medications have been studied extensively. The most common side effects are gastrointestinal — nausea, vomiting, diarrhea, and constipation — especially when starting or increasing the dose. These usually improve over time.
More serious but rare risks include:
- Pancreatitis (inflammation of the pancreas)
- Gallbladder issues
- Rare thyroid tumors (seen in animal studies; risk in humans unclear)
Always discuss your full medical history with your doctor before starting any GLP-1 treatment.
How Are GLP-1 Injections Given?
Most injectable GLP-1 medications come in pre-filled auto-injector pens. They’re typically injected once weekly into the abdomen, thigh, or upper arm. The needles are very small and thin — many people find them much less intimidating than they expected.
Do You Have to Stay on Them Forever?
This is one of the most common questions. Research shows that stopping GLP-1 medications often leads to weight regain — similar to stopping any chronic disease treatment. Most medical guidelines now treat obesity as a chronic condition requiring long-term management, which means ongoing treatment for many patients.
Conclusion: Is a GLP-1 Injection Right for You?
GLP-1 injections have genuinely changed the landscape of diabetes care and weight management. The science is clear: these medications work by mimicking a natural hormone to regulate blood sugar, slow digestion, reduce appetite, and — increasingly — protect the heart.
With over 30 million Americans already using them and new, more powerful options arriving in 2026, access and effectiveness are only improving.
✅ Actionable Next Steps
- Talk to your doctor — Ask whether a GLP-1 medication fits your health profile, especially if you have type 2 diabetes, obesity, or cardiovascular risk factors.
- Understand your options — Injectable and oral forms are now available. Discuss which format suits your lifestyle.
- Check your insurance — Coverage varies widely. Ask your pharmacist or insurer about GLP-1 coverage and patient assistance programs.
- Pair with lifestyle changes — Clinical trials combine these medications with diet and exercise. The best results come from a whole-health approach.
- Stay informed — With multiple FDA decisions expected in 2026, new and potentially more effective options may soon be available.
GLP-1 therapy isn’t a magic fix, but for many people, it’s the closest thing to one that modern medicine has produced. The key is working with a qualified healthcare provider to find the right treatment plan for you.
References
[1] GLP-1 Pipeline Update February 2026 – https://www.primetherapeutics.com/glp-1-pipeline-update-february-2026
[2] GLP-1 Pills for Weight Loss Are Here: How Will They Change Obesity Care – https://www.aamc.org/news/glp-1-pills-weight-loss-are-here-how-will-they-change-obesity-care
[3] GLP-1 Trends – https://www.goodrx.com/classes/glp-1-agonists/glp-1-trends
[4] What’s Next for GLP-1s – https://news.harvard.edu/gazette/story/2026/02/whats-next-for-glp-1s/
[5] Everything You Need to Know About GLP-1s for Weight Loss – https://pharmaceutical-journal.com/article/feature/everything-you-need-to-know-about-glp-1s-for-weight-loss
[6] GLP-1 Weight Loss Drugs Comparably Effective for Patients Across Age, Race, and Starting Weight – https://publichealth.jhu.edu/2026/glp-1-weight-loss-drugs-comparably-effective-for-patients-across-age-race-and-starting-weight
[7] Outlook for Obesity in 2026 – https://www.iqvia.com/locations/emea/blogs/2026/01/outlook-for-obesity-in-2026
Medical Disclaimer: The information on https://healthfactsjournal.com is for educational and informational purposes only and is not intended as medical advice. These statements have not been evaluated by the FDA. Always seek the advice of a qualified healthcare provider regarding any medical condition or treatment. Never disregard professional medical advice or delay seeking it because of something you have read on this website.






