How to Appeal Insurance Denial for Semaglutide: A 2026 Step-by-Step Guide

If you just received a letter saying your semaglutide prescription was denied, you aren’t alone. In early 2026, nearly 56% of commercial insurance plans now have “Restricted” or “No Coverage” policies for weight-loss medications.
However, data shows that approximately 44% of denials are successfully overturned upon appeal. This detailed guide on How to Appeal Insurance Denial for Semaglutide, explain how to build a case that your insurer cannot ignore.
Quick Answer: If your insurer denied coverage for semaglutide (Ozempic, Wegovy, or Rybelsus), you have the legal right to appeal — and it’s worth doing. Approximately 44% of insurance denials are successfully overturned on appeal, with success rates climbing above 65% when you submit proper documentation [1][9]. The process involves up to three levels: an internal appeal, an external independent review, and a state insurance commissioner complaint.
Key Takeaways
- 📋 You typically have 180 days from your denial date to file an appeal — don’t wait [1][4].
- 🏥 A detailed Letter of Medical Necessity from your doctor is the single most important document in your appeal [2][6].
- 📊 Internal appeals succeed 20–30% of the time; external reviews succeed 40–50% of the time [2][9].
- 💊 Document every prior medication tried (Phentermine, Metformin, Orlistat) with dates, dosages, and outcomes [4].
- 🔢 Use the correct ICD-10 diagnosis codes — your doctor must match them to your specific condition (obesity, Type 2 diabetes, cardiovascular risk) [4][5].
- ⚡ For urgent medical situations, request an expedited review — decisions must come within 72 hours [2][4].
- 🏛️ If internal and external appeals both fail, file a complaint with your state insurance commissioner [2].
- 💰 If coverage is ultimately denied, semaglutide without insurance costs and savings strategies can help you find affordable alternatives.
Why Do Insurers Deny Semaglutide in the First Place?
Insurance companies deny semaglutide for a handful of predictable reasons. Knowing exactly why you were denied is the foundation of a successful appeal — because your appeal must directly address the stated reason.
The most common denial triggers include [1][2][4]:
- Lack of medical necessity documentation — the insurer doesn’t have enough clinical evidence that semaglutide is required for your specific condition.
- Step therapy requirements not met — your plan requires you to try and fail cheaper medications first (such as Metformin, Phentermine, or Orlistat).
- Plan exclusion — some employer-sponsored plans explicitly exclude weight loss medications, even FDA-approved ones.
- Missing or incorrect diagnosis codes — if your doctor submitted the wrong ICD-10 code, the claim may be auto-denied.
- BMI or comorbidity thresholds not documented — many plans require a BMI of 30+ (or 27+ with a qualifying condition) to be clearly stated in the record.
Read your denial letter carefully. Insurers are legally required to explain the specific reason for denial. That reason is your roadmap for the appeal.
Common mistake: Many patients submit a generic appeal without addressing the insurer’s stated reason. If the denial says “step therapy not satisfied,” your appeal must show exactly which medications you tried, for how long, and why they didn’t work [4].
Step 1: Decode the Denial Reason
Before you write a word, you must know why they said “No.” Look at your Explanation of Benefits (EOB) for these common 2026 denial codes:
- “Not Medically Necessary”: The insurer believes you haven’t tried cheaper alternatives (Step Therapy) or don’t meet the BMI/comorbidity threshold.
- “Plan Exclusion”: The most difficult to fight. This means your employer specifically chose a plan that does not cover weight-loss drugs.
- “Step Therapy Required”: They want you to try older, cheaper medications (like Phentermine or Contrave) for 3–6 months first.
Step 2: Leverage the “2026 Comorbidity” Strategy
In 2026, insurers are more likely to approve semaglutide if it is prescribed for something other than just “weight loss.” If you have any of the following, ensure they are the focal point of your appeal:
- MASH (formerly NASH): New 2026 guidelines favor semaglutide for metabolic dysfunction-associated steatohepatitis.
- Cardiovascular Risk: Following the SELECT trial results, Wegovy is FDA-approved to reduce the risk of heart attack and stroke in patients with heart disease and obesity.
- Sleep Apnea: If you use a CPAP machine, emphasize that weight loss is a primary treatment for obstructive sleep apnea (OSA).
Step 3: Gather Your “Evidence Bundle”
A successful appeal is a paper trail. You (and your doctor) should include:
- A Letter of Medical Necessity (LOMN): This must be signed by your provider.
- Lab Results: Current A1c, liver enzymes, and blood pressure readings.
- Historical Effort: A list of “failed” interventions (e.g., “Patient attempted Nutrisystem for 6 months with <3% weight loss”).
- The “Bridge” Clause: If you are a Medicare patient, mention the 2026 Medicare GLP-1 Bridge program if you meet the heart disease or sleep apnea criteria.
Step 4: Write the Appeal Letter
Use the template below to structure your argument. Be objective, concise, and firm.
📝 Sample Appeal Snippet
“I am writing to formally appeal the denial of [Medication Name] (Claim #12345). While this medication is indicated for weight management, it is being prescribed as a critical intervention for [Your Specific Condition, e.g., Stage 2 Liver Fibrosis or Cardiovascular Disease Prevention]. Clinical data from 2025/2026 trials demonstrate that for patients in my profile, semaglutide reduces the long-term risk of [Heart Attack/Liver Failure], which represents a significantly higher cost-burden to [Insurance Company Name] than the monthly cost of this therapy.”
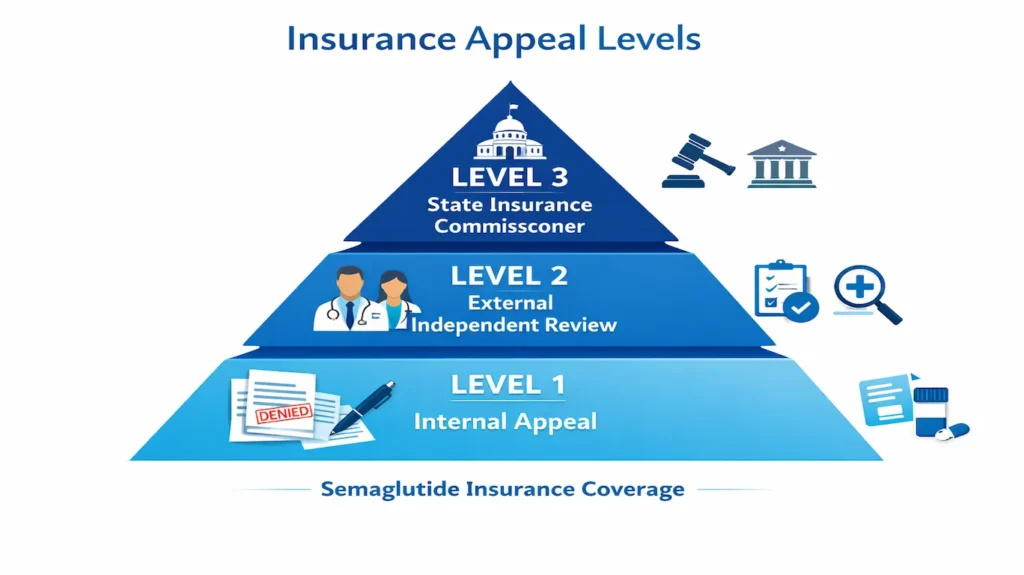
What Are the Three Levels of a Semaglutide Insurance Appeal?
The appeal process for semaglutide insurance coverage follows a structured three-level system. Each level gives you a stronger, more independent review of your case.
Level 1: Internal Appeal
You file this directly with your insurance company. Submit a written request within your plan’s deadline (typically 180 days from the denial date) [1][4]. Include:
- A formal appeal letter addressing the denial reason point by point
- A Letter of Medical Necessity from your prescribing physician
- Supporting medical records (BMI, lab results, diagnosis, comorbidities)
- Evidence of prior treatments tried and failed
Standard internal appeals take 30 days for prior authorization requests and 60 days for services already received [2][4].
Success rate: 20–30% [2][9]
Level 2: External Independent Review
If the internal appeal fails, you can request an external review. An independent medical professional — with no financial ties to your insurer — reviews your case based purely on clinical evidence [2]. These reviewers often have direct experience with GLP-1 medications and tend to apply clinical standards rather than insurance plan language.
External reviews take up to 60 days [2].
Success rate: 40–50% [2][9]
Level 3: State Insurance Commissioner
If both previous levels fail, file a formal complaint with your state’s insurance commissioner. Regulators can investigate whether your insurer followed proper procedures and may mediate the dispute [2]. This process can take 90 days or longer.
Choose Level 3 if: You believe your insurer violated state insurance regulations or failed to follow proper appeal procedures.
What Documentation Do You Need for a Strong Appeal?

Strong documentation is what separates successful appeals from failed ones. According to available data, appeals with complete, targeted documentation succeed at rates above 65% [1][9].
Here’s what to gather before you file:
Essential Documents Checklist
| Document | What to Include |
| Denial Letter | The exact reason for denial (required by law) |
| Letter of Medical Necessity | Physician-authored, diagnosis-specific, and detailed |
| Medical Records | BMI measurements, lab results, and recent visit notes |
| ICD-10 Codes | Must match your specific condition (Obesity, T2D, CVD risk) |
| Step Therapy Records | Prior medications, dates, dosages, and outcomes |
| Lifestyle Intervention Proof | Gym memberships, dietitian visits, or program enrollment |
| Clinical Guidelines | ADA, AACE, or Obesity Society recommendations |
The Letter of Medical Necessity: What It Must Say
Your doctor’s letter is the most critical piece of your appeal [2][6]. A weak, generic letter is one of the top reasons appeals fail. The letter should:
- State your specific diagnosis and relevant ICD-10 code(s)
- Explain why semaglutide is medically necessary for your case (not just generally useful)
- Document your BMI and any comorbidities (Type 2 diabetes, hypertension, sleep apnea, cardiovascular risk)
- List every alternative treatment tried, with dates and documented failure
- Reference current clinical guidelines supporting GLP-1 therapy
- Address the insurer’s specific denial reason directly
For patients using semaglutide for Type 2 diabetes, see our complete guide to semaglutide for Type 2 diabetes for clinical context your doctor can reference.
Step Therapy Documentation
If your denial involves step therapy, you need detailed records for each prior medication [4]:
- Drug name, dose, and duration
- Side effects experienced
- Lack of clinical response (with objective data where possible)
- Reason for discontinuation
Acceptable prior medications often include Phentermine, Metformin, Orlistat, and Topiramate. Lifestyle programs like Weight Watchers or medically supervised diet programs also count — include enrollment dates and participation records [4].
The 3 Most Affordable GLP 1 Without Insurance (2026 Ranked)
While GLP-1 receptor agonists have dominated the headlines recently, the 2026 shift in obesity medicine is moving toward ‘precision prescribing.’
As Dr. Fitch notes, we have a deep clinical history with non-injected therapies that predates the Ozempic era. For patients who don’t tolerate semaglutide or have specific ’emotional eating’ triggers, oral combinations like DirectMeds or MyStart GLP-1 remain highly effective, science-backed pillars of metabolic health.”
🥇 #1 Best Overall: Zepbound (Triple-Action Option)

🥇 Best Overall (9.9/10)
DirectMeds GLP1 provides a budget-friendly alternative to Ozempic/Wegovy while maintaining strong appetite control and weekly fat loss results. Everything is included—from telehealth visits to medication shipping—making it ideal for people wanting premium results at the lowest cost.
DirectMeds is a LegitScript-certified telehealth platform that connects patients with licensed U.S. physicians who evaluate whether compounded GLP-1 medications are clinically appropriate.
It is one of the most established providers in this space and is particularly well-suited to patients who want high-touch clinical oversight without paying brand-name prices.
How it works: Complete a secure online health intake form. A licensed medical provider reviews your profile and determines eligibility. If approved, your prescription is sent to a certified U.S. compounding pharmacy and medication is shipped directly to your door. All-inclusive pricing covers medical consultation, medication, and 24/7 support — no surprise charges.
◉ Clinical Note: DirectMeds’ LegitScript certification is a meaningful differentiator in this market. It requires compliance with pharmacy laws, prescription standards, and advertising guidelines — reducing the risk of receiving substandard compounded medications. For patients new to telehealth GLP-1 programs, this certification provides a meaningful layer of accountability. — Dr. Sarah Jenkins, Co-Author
🎯 Ideal for: Patients who want an established, verified provider with strong clinical support and are comfortable paying slightly more than the absolute floor price for greater peace of mind.
🥈#2 Best for Long-Term Cost Certainty: MyStart GLP-1
🥈 Silver Standard — Best Flat-Rate Pricing

- Rating: ⭐️⭐️⭐️⭐️⭐️ – (9.9/10) High Potency GLP1
MyStart GLP-1 offers a smooth, beginner-friendly GLP-1 program using FDA-backed medications and simple weekly injections or tablets. Great for people wanting easy onboarding, rapid fat loss, and physician oversight—without the high price of traditional clinics.
MyStart GLP-1 uses a unique flat-rate membership model where your medication cost is fixed regardless of how high your therapeutic dose increases over time. For patients who will be on GLP-1 therapy for 12 months or more, this pricing structure can save $600 to $1,800 annually compared to platforms that charge progressively more as doses escalate.
How it works: Pay a monthly membership ($79) plus a flat medication fee (e.g., $175 for compounded semaglutide). The combined total stays fixed at $254 per month from starter dose through maximum maintenance dose. Medical consultation, all medication, dedicated care team access, and nutritional coaching are included.
◉ Clinical Note: The flat-rate model is financially sound for long-term GLP-1 use. GLP-1 therapy is most effective when sustained for 12+ months, and avoiding dose-related price increases removes a common reason patients discontinue treatment early. The included nutritional coaching adds meaningful clinical value, as sustainable weight loss requires both medication and lifestyle change. — Dr. Sarah Jenkins, Co-Author
🎯 Ideal for: Patients committed to long-term treatment (12+ months) who want price certainty as doses increase, and who value behavioral coaching as part of their program.
Best for: People who want a more advanced GLP-1 approach at a reduced price. 👉 SKIP THE WAITLIST. START FOR $199
Thousands of people are losing weight with MyStart GLP-1 medications. People like you are transforming their lives, feeling better, and looking their best with the help of GLP-1 (Dual-Action Option) medications.
🥉 #3 Best for Absolute Lowest Entry Cost: MEDVi GLP-1
🥉 Bronze Standard — Lowest Entry Price

- Rating: ⭐️⭐️⭐️⭐️⭐️ – (9.9/10) Excellent
MEDVi GLP-1 delivers fast, medical-grade weight loss with doctor-guided dosing and personalized coaching. Patients report losing 1–3 lbs per week with steady appetite control and reduced cravings. Qualify in minutes and access 600+ U.S. doctors with no membership fees.
MEDVi offers the most accessible entry price point in the compounded GLP-1 market, with starter doses beginning as low as $99 per month and a published price-match guarantee.
The platform provides both injectable and oral compounded GLP-1 options, giving prescribers flexibility to match the medication form to the patient. Clinical follow-up is primarily quarterly rather than monthly, which keeps costs lower but means less frequent dose adjustment guidance than the two options above.
How it works: Complete an online consultation. If qualified, your prescription is sent to a partner compounding pharmacy and medication is shipped to you within 48 hours. Customer support is available, and clinical check-ins are typically quarterly. No membership fees are charged on top of medication pricing.
◉ Clinical Note: MEDVi is a legitimate, cost-effective option for budget-focused patients who have researched compounded medications and are comfortable with less frequent clinical contact. Always ask your provider which specific compounding pharmacy fulfills your prescription — a reputable 503A or 503B state-licensed pharmacy is non-negotiable for safety. — Dr. Sarah Jenkins, Co-Author
🎯 Ideal for: Budget-focused patients who have done their research on compounded GLP-1 medications, are comfortable managing more of their own care independently, and want the lowest possible entry price with a price-match guarantee.
How Do You Write an Effective Appeal Letter?
A well-written appeal letter is direct, organized, and clinical in tone. It does not plead — it presents evidence. Here’s the structure that works:
- Opening paragraph: State that you are appealing the denial dated [X] for [medication/brand name], and reference your claim or case number.
- Restate the denial reason: Show the insurer you understand exactly why they denied coverage.
- Address each denial reason with evidence: One section per reason, with supporting documentation cited.
- Medical necessity argument: Summarize why semaglutide is the appropriate, evidence-based treatment for your condition.
- Cost-savings argument (optional but effective): For plan exclusion denials, note that treating obesity-related comorbidities costs significantly more long-term than covering the medication [1].
- Closing: Request a specific outcome (approval of coverage), provide your contact information, and list all enclosed documents.
Edge case — plan exclusions: If your plan explicitly excludes weight loss medications, a standard medical necessity argument may not be enough. In this situation, frame your appeal around the medical diagnosis (obesity as a chronic disease, or cardiovascular risk reduction) rather than weight loss as a goal [1][8].
Some patients have succeeded by having their physician document the cardiovascular indication rather than the weight management indication.
What Are the Key Timelines You Must Know?
Missing a deadline is one of the most common — and most avoidable — reasons appeals fail. Here are the timelines that apply to most health plans [2][4]:
- Filing deadline: 180 days (6 months) from the denial date
- Internal appeal decision: 30 days (prior auth) or 60 days (post-service)
- Expedited review: 72 hours for urgent pre-service; 24 hours for concurrent care
- External review: Up to 60 days
- State commissioner complaint: 90+ days
⚡ Request an expedited review if your condition is urgent — for example, if delayed treatment poses a significant health risk. Insurers must respond within 72 hours [2][4].
Plans created after March 23, 2010 are required by federal law to allow internal and external appeals under the Affordable Care Act [1][4].
Step 5: The External Review (The “Final Boss”)
If your insurance company denies your internal appeal, you have the right to an Independent External Review.
- This is conducted by a third-party medical professional who does not work for the insurance company.
- In 2026, external reviewers are increasingly siding with patients, especially for those with “high-risk” comorbidities.
- Timeline: You usually have 180 days from the final denial to request this.
🛠️ What if the Appeal Fails?
If you hit a brick wall, don’t pay the $1,300 retail price. In 2026, you have these backup options:
- Manufacturer Patient Assistance Programs (PAP): If you are uninsured or have Medicare, check NovoCare; they often provide the drug for $0 if you meet income requirements.
- DTC “Cash” Pricing: Use manufacturer-direct portals which have dropped prices to $349/month to compete with generics.
- The “Generic” Shift: As of early 2026, keep an eye on Canadian and Indian generic arrivals (like Obeda), which are beginning to influence US “coupon” pricing.
What If Your Appeal Is Denied at Every Level?
If all three appeal levels fail, you still have options. A denied appeal is not the end of the road for accessing semaglutide.
Alternative paths to consider:
- Manufacturer savings programs: Novo Nordisk offers savings cards for Ozempic and Wegovy for eligible commercially insured patients. Check the manufacturer’s website directly for current eligibility.
- Compounding pharmacies: Compounded semaglutide has been available through telehealth providers, though regulatory status changes frequently — verify current FDA guidance before pursuing this route.
- Telehealth and direct-pay programs: Several telehealth platforms offer semaglutide at reduced cash-pay prices. Our guide to affordable GLP-1 options without insurance covers current pricing from $199/month.
- Switch medications: If tirzepatide (Mounjaro/Zepbound) has better coverage under your plan, it may be worth discussing with your doctor. See our semaglutide vs. tirzepatide comparison for clinical differences.
- Open enrollment: If your employer offers multiple plan options, review GLP-1 coverage before your next open enrollment period.
For a full breakdown of what you’d pay out of pocket, our semaglutide cost breakdown with and without insurance covers 2026 pricing across all major brands.
Frequently Asked Questions: How to Appeal Insurance Denial for Semaglutide
Q: How long does a semaglutide insurance appeal take? Internal appeals take 30–60 days for standard requests and 72 hours for expedited urgent reviews. External reviews take up to 60 days. Plan for 2–4 months if you go through all levels [2][4].
Q: Can my doctor help me appeal? Yes — and your doctor’s involvement is critical. A detailed Letter of Medical Necessity from your physician is the strongest single document in any appeal [2][6]. Ask your doctor’s office if they have experience writing appeal letters for GLP-1 medications.
Q: What ICD-10 codes support a semaglutide appeal? Common codes include E11 (Type 2 diabetes mellitus), E66 (obesity), Z68 (BMI codes), and I10 (hypertension). Your doctor should select the code(s) that most accurately reflect your diagnosis and the indication for treatment [4][5].
Q: Does Medicare cover semaglutide? Medicare Part D covers Ozempic for Type 2 diabetes. As of 2026, coverage for Wegovy (the weight management indication) under Medicare has expanded following legislative changes — confirm your specific plan’s formulary, as coverage varies [7][10].
Q: What if my employer plan excludes weight loss drugs entirely? You can still appeal by framing the medication around a covered medical diagnosis (such as Type 2 diabetes or cardiovascular risk reduction) rather than weight loss. If the exclusion is absolute, your best options are manufacturer savings programs or direct-pay telehealth providers [1][8].
Q: Is there a fee to request an external review? Federal law limits external review fees to $25 or less per request for most plans. Many states require external reviews to be free [2].
Q: What’s the difference between Ozempic and Wegovy for insurance purposes? Both contain semaglutide, but they are FDA-approved for different indications. Ozempic is approved for Type 2 diabetes; Wegovy is approved for chronic weight management. Insurers treat them differently, and coverage criteria vary significantly. See our semaglutide brand names guide for a full comparison.
Q: Can I appeal if my insurer stopped covering semaglutide mid-treatment? Yes. Mid-treatment coverage terminations are appealable. Document your treatment history, clinical response, and any evidence that stopping the medication would harm your health [7][10].
Q: Should I hire a patient advocate? For complex cases — especially plan exclusions or repeated denials — a patient advocate or healthcare attorney can significantly improve your odds. The Obesity Action Coalition offers free resources for navigating obesity medication appeals [8].
Q: What if I need semaglutide now and can’t wait for the appeal? Ask your doctor about manufacturer patient assistance programs or check how to get semaglutide through alternative providers while your appeal is pending.
Conclusion On How to Appeal Insurance Denial for Semaglutide
Appealing a semaglutide insurance denial is a real, winnable process — not a bureaucratic dead end. The data is clear: with proper documentation and a targeted appeal letter, your odds of overturning a denial improve substantially [1][9].
Your action plan:
- Read your denial letter today and identify the exact stated reason.
- Call your doctor’s office and request a detailed Letter of Medical Necessity that addresses that specific reason.
- Gather all supporting documents — medical records, step therapy history, lifestyle intervention proof, and ICD-10 codes.
- File your internal appeal within 180 days of the denial date.
- If denied internally, request an external independent review immediately.
- If all else fails, file a state insurance commissioner complaint and explore direct-pay options in the meantime.
Don’t let one denial letter be the final word. Semaglutide insurance coverage is worth fighting for — and the process gives you multiple legitimate opportunities to win.
References
[1] Drugs How To Appeal Wegovy Denial – https://www.medicalnewstoday.com/articles/drugs-how-to-appeal-wegovy-denial
[2] Appeal Letters Wegovy – https://amazing-meds.com/appeal-letters-wegovy/
[3] GLP-1 Insurance Denials: What To Do – https://www.oanahealth.com/post/glp-1-insurance-denials-what-to-do
[4] GLP-1 Insurance Denials 2026 Coverage Appeals Guide – https://www.globalmedship.com/blogs/medicine-guide/glp-1-insurance-denials-2026-coverage-appeals-guide
[5] Appealing A Denial – https://www.obesityaction.org/action-through-advocacy/access-to-care/access-to-care-resources/appealing-a-denial/
[6] Insurance Stopped Covering My GLP-1 – https://www.singlecare.com/blog/insurance-stopped-covering-my-glp-1/







