Why Am I Hungry All The Time? The Science Behind “Food Noise” (And How To Fix It)

If you constantly think about food, crave sugar after meals, or feel hungry right after eating, you’ve likely asked yourself: “why am i hungry all the time?” The frustrating truth is that traditional advice—”just eat less” or “exercise more”—fails because it ignores the underlying biology.
Constant hunger is often a symptom of metabolic dysfunction: low GLP-1 levels, ghrelin resistance, or a dysregulated dopamine reward system. In this guide, we break down the four biological culprits behind Food Noise and explain how GLP-1 medications are helping thousands of people finally regain control over their appetite.
This article reviews the latest peer-reviewed studies to explain why you never feel full and what science-backed solutions exist—including the role of GLP-1 medications in silencing what doctors now call “Food Noise.”
What Is Food Noise? A Clinical Definition
Food Noise is a term that has recently entered the mainstream lexicon, largely thanks to the rise of GLP-1 medications. However, the phenomenon has existed forever.
According to recent research published in Nutrition & Diabetes, food noise involves “constant preoccupation with food-related decisions—such as which foods to eat, caloric intake, macronutrient balance, and meal timing—which can become intrusive and unpleasant.”
Researchers have now formally defined food noise as “persistent thoughts about food that are perceived by the individual as being unwanted and/or dysphoric and may cause harm to the individual, including social, mental, or physical problems.”
Food Noise is distinguished from routine food-related thoughts by its intensity and intrusiveness, resembling rumination. It affects cognitive burden and quality of life, and is being cited as one reason weight-loss attempts fail.
For people who do not struggle with this, it sounds exaggerated. They eat when they are hungry and stop when they are full. The thought of food doesn’t dominate their mental real estate.
But for those with metabolic dysfunction, Food Noise is a 24/7 radio station playing in the background of their minds—and they can’t find the off switch.
The Difference Between Physical Hunger and Food Noise
It is crucial to distinguish between true hunger and Food Noise:
| Physical Hunger | Food Noise |
|---|---|
| Comes on gradually | Comes on suddenly |
| Happens 4-5 hours after a meal | Happens right after a meal |
| Any food sounds good | Craves specific foods (sugar, salt, fat) |
| Stops when full | Continues even when full |
| Located in the stomach | Located in the mind |
If you are tired of fighting the noise, explore your options for GLP-1 therapy today.
👉 See how much you could save: [Most affordable GLP-1 Without Insurance (Updated 2026)]

Why Am I Hungry All The Time? The 4 Biological Culprits
If you are constantly hungry or plagued by Food Noise, one of these four biological systems is likely malfunctioning. These findings are supported by extensive research into neurohormonal appetite control.
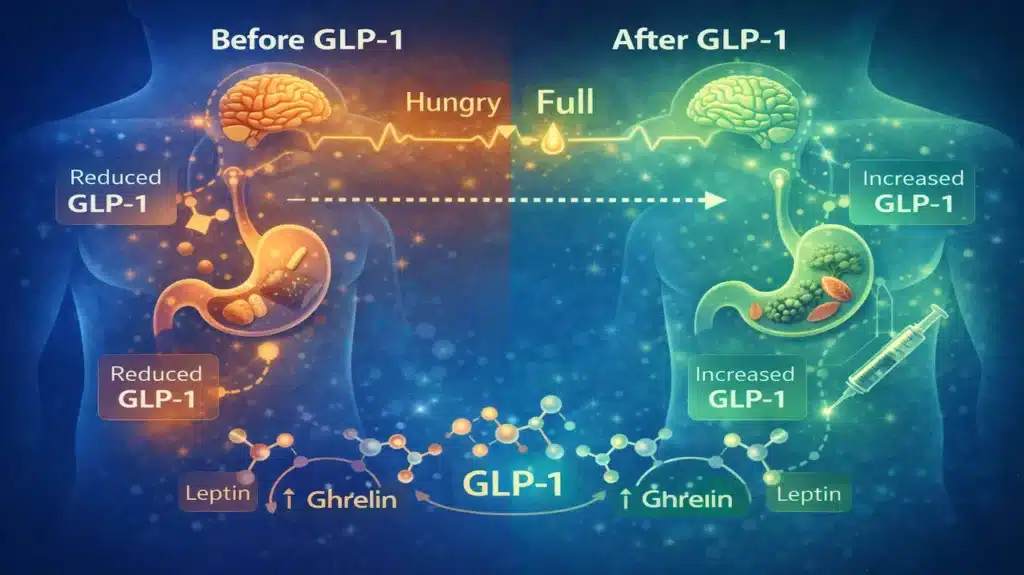
Culprit #1: The GLP-1 Deficiency (The Missing Brakes)
GLP-1 (glucagon-like peptide-1) is an incretin hormone secreted by enteroendocrine L-cells in the gut and acts on the hypothalamus to regulate appetite.
- How it works: When you eat, your intestines release GLP-1. This hormone slows down gastric emptying and travels to the brain to suppress appetite. GLP-1 increases the expression of cAMP, PKA, and CREB metabolic pathways in the central nervous system.
- The Problem: In many individuals—particularly those with insulin resistance, prediabetes, or obesity—the body either doesn’t secrete enough GLP-1, or the brain becomes resistant to its signals. GLP-1 receptors are present in different brain regions including the hypothalamus, where they influence appetite control and satiety.
- The Result: The “I’m full” signal never arrives. Food passes through your system too quickly, leaving you hungry again soon after eating.
Culprit #2: The Ghrelin Spike (The Screaming Accelerator)
Ghrelin, termed the “hunger hormone,” was initially discovered through its receptor, the growth hormone secretagogue receptor (GHS-R), before researchers explained its role as a growth-hormone-releasing peptide.
- How it works: Ghrelin is a 28-amino acid peptide synthesized from the human ghrelin gene (GHRL) on chromosome 3. X/A-like cells in the gastric tissue are the primary synthesizing cells. Ghrelin levels typically rise before a meal (making you feel hungry) and drop after a meal (making you feel satisfied). The lateral area of the hypothalamus is responsible for hunger and becomes stimulated by ghrelin.
- The Problem: Research shows that some people with obesity do not experience the same post-meal drop in ghrelin. Their levels stay high, meaning their brain continues to receive “EAT” signals even after consuming adequate calories.
- The Result: You feel hungry immediately after eating because your hormones are still screaming for fuel. Circulating ghrelin acts on the lateral hypothalamus, and this region has also been shown to form and store memories associated with predicting food availability.
Culprit #3: The Blood Sugar Rollercoaster
What you eat directly impacts your hunger levels through glucose homeostasis mechanisms.
- The Cycle: You eat refined carbohydrates (pasta, bread, sugar). Your blood sugar spikes rapidly. Your pancreas releases a surge of insulin to deal with the sugar. GLP-1 plays a crucial role here—it promotes glucose-dependent insulin secretion and inhibits glucagon release from pancreatic α-cells.
- The Crash: Low blood sugar (reactive hypoglycemia) is perceived by your body as a life-threatening emergency. It triggers intense cravings for quick energy—usually more sugar or carbs. GLP-1 receptor agonists like semaglutide and liraglutide help stabilize this by improving glucose homeostasis and reducing blood sugar variability.
- The Result: You are stuck in a vicious cycle of spikes and crashes, with the crashes driving you to eat every 2-3 hours.
Culprit #4: The Dopamine Loop (The Brain Reward System)
Sometimes, hunger isn’t about energy—it’s about pleasure. This is where Food Noise overlaps with addiction science.
- The Mechanism: According to the Oxford Handbook of Food & Addiction, reward can be parsed into separate psychological features: “wanting” and “liking.” Motivation to pursue and consume rewards (‘wanting’) is largely mediated by brain dopamine and other neuropeptides within mesocorticolimbic circuitry.
- The Adaptation: Highly palatable foods (high in sugar, fat, and salt) trigger the release of dopamine in the brain’s reward center. The incentive sensitization theory of addiction proposes that neural adaptations increase ‘wanting’ over time, while ‘liking’ stays relatively the same. Highly palatable foods may cause similar neural and behavioral sensitization.
- The Result: You crave ice cream not because you need calories, but because your brain is seeking a dopamine reward. The consumption of ultra-processed food activates your hedonic pathway or reward pathway—processed food gives you a reward, and a reward means you want to keep going back.
The Role of Leptin in Satiety
Leptin is perhaps best understood as the opposite of ghrelin, acting as the body’s satiety signal. The obese (ob) gene, located on chromosome 7, produces leptin, which is primarily found in adipose tissues.
Leptin is an adipocyte-derived hormone existing as a 167 amino acid peptide. It is released into the bloodstream as a function of adipose storage, signaling the brain to regulate homeostasis. The ventromedial region of the hypothalamus is responsible for satiety and is stimulated by leptin. Furthermore, leptin inhibits stimulation of the lateral hypothalamus to inhibit the effects of ghrelin.
Subjects with a higher BMI and corresponding percent of body fat have demonstrated a marked increase of leptin in the circulating blood plasma—a condition known as leptin resistance, where the brain no longer responds properly to satiety signals.
“Ready to silence the food noise? See the latest pricing and savings options for GLP-1 medications in our 👉 [Cheapest GLP-1 Without Insurance (Updated 2026)] guide.”
Real Questions from People Like You
To truly understand Food Noise, let’s look at the questions real people are asking online. If any of these resonate, you are in the right place.
Query: “Why do I crave sugar at night?”
The Science: Late-night cravings are often a combination of dopamine-seeking behavior (rewarding yourself for getting through the day) and blood sugar instability from dinner. The endocannabinoid system also shows natural circadian rhythm variations that may increase reward-seeking in the evening. GLP-1 agonists have been shown to reduce these cravings by acting on reward pathways.
Query: “Why do I think about food as soon as I wake up?”
The Science: Morning hunger can be driven by high overnight ghrelin production or the “dawn phenomenon,” a natural rise in blood sugar that occurs in the early morning hours. Ghrelin is also involved in regulating sleep-wake rhythms, which may explain this phenomenon.
Query: “Why am I never full?”
The Science: As discussed under Culprit #1, this is almost certainly a GLP-1 or leptin signaling deficiency. Your stomach may be stretched, but your brain never received the signal to stop eating. The arcuate nucleus of the hypothalamus integrates signals from both hormones, and disruption here affects overall energy balance.
Query: “Why do I eat when I’m stressed?”
The Science: Cortisol (the stress hormone) increases appetite, particularly for “comfort foods” high in sugar and fat. This is an ancient survival mechanism—in times of stress, the body craves high-energy fuel. GLP-1 receptors are present in areas of the brain that regulate stress response, and GLP-1 agonists have been shown to modulate these pathways.
The “Stomach vs. Brain” Disconnect
One of the most frustrating aspects of Food Noise is the disconnect between the stomach and the brain.
You can feel physically full—even uncomfortably stuffed—yet still feel the urge to eat.
This is the ultimate proof that Food Noise is neurological, not physical. Your stomach is sending signal “A” (I am full of food), but your brain is receiving signal “B” (I need dopamine / I am stressed / I am bored).
This disconnect is the primary reason why “eating less” fails as a long-term strategy. You are trying to solve a brain problem with a stomach solution.
The hypothalamus acts as the key central integrator of various hunger signals from the body. Within the hypothalamus are specific regions where hormones interact to produce sensations of appetite and satiety. Through the interactions of ghrelin and leptin, the hypothalamus regulates the sensation of hunger and satiety, leading to energy homeostasis.
“Stop fighting your biology. Connect with a licensed provider today and discover affordable GLP-1 options through
👉[TrumpRx vs Private Telehealth: Where Is GLP-1 Cheaper?].”
How to Stop Food Noise

If you have read this far, you know that willpower is not the answer. So what is?
Here are the three primary ways to address Food Noise, ranked from lifestyle to medical intervention.
Level 1: Dietary Adjustment
You can attempt to stabilize your blood sugar and hunger hormones through diet:
- Increase Protein: Protein is the most satiating macronutrient. It increases GLP-1 and reduces ghrelin naturally. Aim for 30g of protein per meal.
- Fiber: Soluble fiber slows digestion and helps regulate blood sugar.
- Eliminate Spikes: Remove or drastically reduce refined sugar and white flour to prevent the blood sugar crashes that trigger cravings.
- Eat Intentionally: “You want to eat on time and eat intentionally. Why is that important? Because food is fuel for the body. If you don’t get fuel, your body’s metabolic rate will slow down.”
The Limitation: For those with significant metabolic dysfunction, diet alone often isn’t enough to override a deficient GLP-1 system.
“Not all GLP-1s are created equal. Find out which medication ranks #1 for appetite suppression in our [Best GLP-1 for Appetite Suppression (Ranked by Effectiveness)] comparison.”
Level 2: Lifestyle Modification
- Exercise: Building muscle mass helps regulate insulin sensitivity and appetite hormones. An exercise physiologist can work with you and any limitations to help you move and strengthen muscle groups.
- Sleep: Sleep deprivation increases ghrelin and decreases leptin. Studies show that sleep-deprived individuals consume an average of 300 more calories per day. “If you’re not getting a good quality, restful sleep, it becomes very hard to adopt healthy lifestyles. When you’re tired or fatigued, you tend to gravitate toward processed and ultra-processed foods.”
- Stress Reduction: “Focus on managing your stressors. This can include talking to a psychologist who can help you deal with emotional hunger.” Other ways to reduce stress can include listening to music, being in nature, or connecting with others.
Level 3: Medical Intervention (GLP-1 Medications)
This is where the modern solution meets the biological problem.
If your body does not produce enough GLP-1, or if your brain does not respond to it, you can supplement it. GLP-1 receptor agonists (like semaglutide, the active ingredient in Ozempic and Wegovy) are synthetic versions of the hormone your body is missing.
How they silence Food Noise:
- They replace the missing signal: Semaglutide and liraglutide bind to GLP-1 receptors in the brain, activating cAMP and PKA signaling cascades. This effectively turns the volume back on for the “I’m full” message.
- They slow the stomach: They slow gastric emptying, creating physical fullness that lasts longer.
- They blunt the reward: GLP-1 receptor agonists act on the brain’s reward centers, reducing the “dopamine hit” you get from junk food. Research shows that GLP-1 can modulate phosphorylation of AKT, ERK, GSK-3B, and mTOR to influence neuronal signaling.
- They reduce inflammation: GLP-1 receptors are present in macrophages, lymphocytes, and monocytes. GLP-1 agonists suppress proinflammatory cytokines such as TNF-α, IL-6, and IL-1β, which may contribute to metabolic improvement.
According to the Cleveland Clinic: “Semaglutide medications tend to activate certain receptors, which promote the release of the hormone GLP-1. GLP-1 tends to decrease your hunger and decrease your appetite. It allows your brain to have much better control over your hunger cues.”
Patients on GLP-1 medications frequently report a phenomenon they describe as “the quiet.”
- “I opened the fridge, looked inside, and closed it. I didn’t want anything. I’ve never done that before.”
- “I forgot to eat lunch. I have never forgotten to eat lunch in my entire life.”
- “The noise is just… gone.”
This is the metabolic reset that diet alone often cannot achieve.
A word of caution: The reduction of cravings is temporary. If you stop taking semaglutides, your cravings are more than likely to return. That’s why it’s important to focus on lifestyle changes that can help you make smarter choices.
The Future of Treatment: Oral GLP-1 Therapies
Recent advances in obesity pharmacotherapy have expanded options beyond injections. According to research published in Cardiovascular Diabetology, two pivotal phase-3 trials of oral GLP-1 therapies were published in September 2025.
- ATTAIN-1 evaluated orforglipron in 3,127 adults with obesity over 72 weeks, demonstrating a mean weight loss of 11.2%, with 54.6% achieving ≥10% weight loss.
- OASIS-4 studied oral semaglutide 25 mg in 307 adults over 64 weeks, showing a mean weight loss of 13.6%, with 63% achieving ≥10% weight loss.
Both agents exhibited gastrointestinal adverse events consistent with the GLP-1 class. These results confirm that oral GLP-1 receptor agonists can produce clinically meaningful weight loss and metabolic benefits, expanding options beyond injectables.
Is It Right for You?
If you identify with any of the following, you may be a candidate for GLP-1 therapy:
- You think about food constantly
- You feel hungry shortly after eating a full meal
- You have tried every diet, only to regain the weight
- You crave sugar and carbs intensely, especially at night
- You have been diagnosed with insulin resistance, PCOS, or prediabetes
- You have a BMI over 30, or over 27 with a weight-related condition
According to endocrinologist Dr. Reena Bose: “If you’re struggling with food noise and it’s impacting your weight, talk to your primary care physician. They can refer you to weight management specialists, which includes obesity medicine physicians, dietitians, exercise physiologists and psychologists—all part of a team who can help customize treatment plans for you.”

“Think you might be a candidate? 👉 Read our [Complete Beginner’s Guide to GLP-1 Weight Loss Injections] to learn how they work, who qualifies, and what to expect.”
Summary: You Are Not the Problem
For decades, society has told people with constant hunger that they lack discipline. We now know that is false.
Constant hunger and intrusive Food Noise are symptoms of a biological system working against you. Whether it’s a GLP-1 deficiency, a ghrelin spike, leptin resistance, or a dopamine-driven reward loop, the problem is chemical, not moral.
The good news? If the problem is chemical, the solution can be chemical, too.
By understanding the science of hunger, you can stop blaming yourself and start exploring real solutions—whether that’s dietary changes, lifestyle optimization, or speaking to a provider about how GLP-1 medications can finally give your brain the “off switch” it has been missing.
Frequently Asked Questions: Why Am I Hungry All The Time?
Is Food Noise the same as binge eating?
Not exactly. Food Noise is the constant, intrusive preoccupation with thoughts of food throughout the day. Binge Eating Disorder (BED) involves consuming large amounts of food in a short period with a feeling of a total loss of control. While persistent Food Noise can often lead to a binge, they are distinct: one is the mental “signal,” and the other is the physical action.
Will drinking more water help with Food Noise?
Sometimes, but usually only temporarily. While it is true that thirst signals can occasionally be mistaken for hunger, true Food Noise is hormonal and neurological in nature. Because it is driven by the brain’s reward system and metabolic signaling, water alone is rarely enough to “silence” the persistent mental urge to eat.
How fast do GLP-1s stop Food Noise?
Many patients report a significant reduction in Food Noise within the first 24 to 48 hours of their first dose. This often happens well before any physical weight loss is visible. This rapid response is consistent with how GLP-1 receptor agonists interact directly with the central nervous system to regulate appetite and reward.
Can I ever stop taking the medication?
For many individuals, Food Noise returns once the medication is discontinued because the underlying metabolic tendency remains. Because obesity is increasingly recognized as a chronic disease, GLP-1 therapy is often viewed as a long-term management tool—much like taking daily medication for high blood pressure or cholesterol.
Are there any risks with GLP-1 medications?
The most common side effects are gastrointestinal, including nausea, vomiting, and diarrhea. These are typically dose-dependent and tend to subside as the body adjusts. While rare, more serious risks like pancreatitis or gallbladder issues can occur, which is why strict medical supervision is essential during treatment.
Does insurance usually cover GLP-1 medications for weight loss?
Coverage varies significantly depending on your specific insurance provider and the underlying diagnosis. While some plans cover these medications for Type 2 Diabetes, others are beginning to add coverage for chronic weight management. It is best to check your plan’s formulary or look for specific clinical criteria required for authorization.
What happens if I miss a dose of my medication?
If you miss a dose, you should typically take it as soon as you remember, provided it is within a few days of the scheduled date (usually 3–5 days depending on the specific brand). If more time has passed, it is often recommended to skip the dose and resume at the next scheduled time. Always consult your healthcare provider or the medication’s guide for the exact protocol for your specific prescription.
Ready to Find Peace?
If you are tired of fighting the noise, explore your options for GLP-1 therapy today.
👉 Compare the top medications: [Best GLP-1 for Appetite Suppression (Ranked)]
Medical References
- Dhurandhar EJ, et al. Food noise: definition, measurement, and future research directions. Nutr Diabetes. 2025. doi: 10.1038/s41387-025-00382-x. PMID: 40628707. Available at: https://pubmed.ncbi.nlm.nih.gov/40628707/
- Young LJ. Ozempic quiets food noise in the brain—but how? Scientific American. 2024. As cited in Dhurandhar EJ, et al. 2025.
- StatPearls. Physiology, Obesity Neurohormonal Appetite And Satiety Control. NCBI Bookshelf. 2024. Available at: https://www.ncbi.nlm.nih.gov/books/NBK555906/
- Warlow SM. The Neuroscience of Food ‘Wanting’ and ‘Liking’. In: Food & Addiction: A Comprehensive Handbook. 2nd ed. Oxford University Press; 2024:245-253. Available at: https://academic.oup.com/book/58145/chapter-abstract/480289046
- López-Gómez JJ, Izaola O, Primo D, de Luis D. Molecular mechanisms of semaglutide and liraglutide as a therapeutic option for obesity. Front Nutr. 2024;11:1398059. doi: 10.3389/fnut.2024.1398059. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11090168/
- Cleveland Clinic. What Is Food Noise? And How To Quiet It. Health Essentials. 2025. Available at: https://health.clevelandclinic.org/food-noise-and-how-to-stop-it
Medical Disclaimer:
This article is for educational purposes only and does not replace professional medical advice. GLP-1 medications require a prescription and medical supervision. Always consult a licensed healthcare provider before starting or changing any treatment.





